Why Medicaid Maps Matter
Call me a geography geek or an atlas addict: I’ve always been a fan of maps. It follows, then, that a recent announcement by the Colorado Department of Health Care Policy and Financing (HCPF) would have me scuttling to my bulletin board and unpinning two of my favorites.
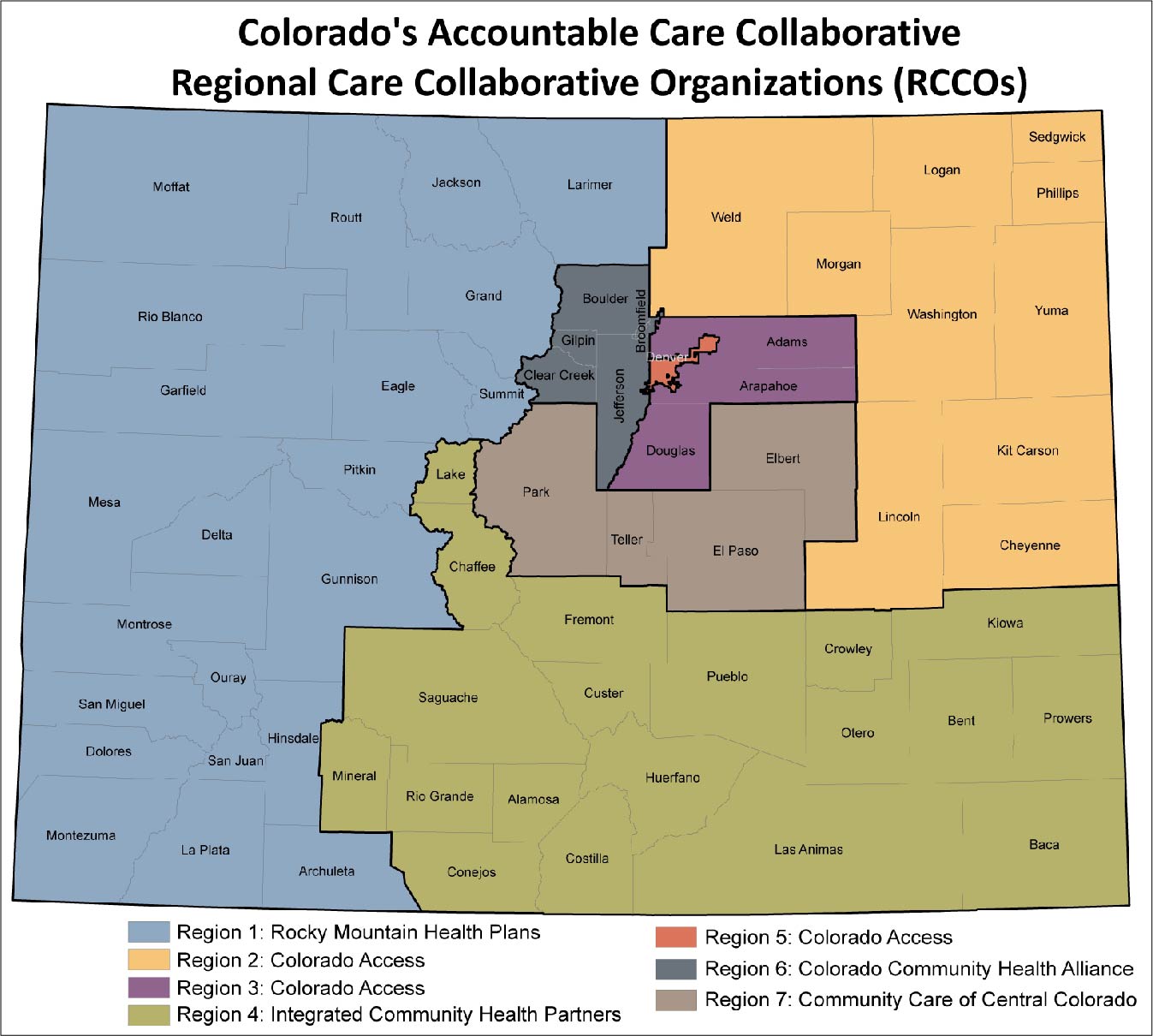
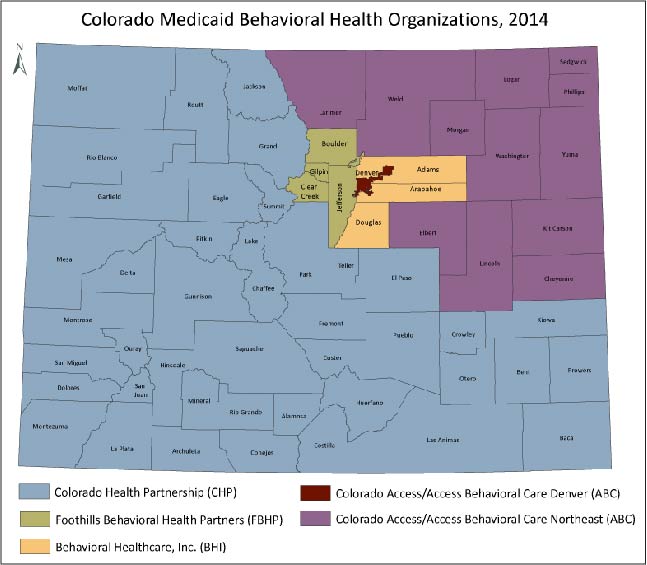
The announcement describes decisions about the future of the Medicaid Accountable Care Collaborative (ACC). The maps shown below display the seven Regional Care Collaborative Organizations (RCCOs) and the five Behavioral Health Organizations (BHOs).
Before we feast on the maps, let’s eat some alphabet soup. The ACC is the state’s big investment in changing how care is delivered to Coloradans enrolled in Medicaid. Within the ACC structure, patients are connected with a medical home where they receive primary and preventive care. The RCCOs are responsible for meeting health and financial benchmarks and ensuring that patient care is coordinated between providers in their regions. Likewise, the five BHOs ensure that Medicaid enrollees in their regions have access to mental health and substance use disorder services.
HCPF’s announcement solidifies the current RCCO map, indicating that the seven regions will not change when new RCCO contracts are awarded in July 2017. It goes a step further, however, indicating that HCPF will contract with only one administrative point of contact to handle the duties historically performed separately by BHOs and RCCOs.
My take is that this doesn’t mean that RCCOs or BHOs are going away, but it may change their business models. And it will definitely mean that many of them will be required to work together in different ways. This makes sense to me when looking at the maps. Most of the BHO regions align exactly with the RCCO regions, except for two counties: Larimer and Elbert. There will be a community engagement process to hammer out the regional assignment of these counties.
What was most interesting to me was HCPF’s decision on payment. Currently, the ACC is built on a fee-for-service structure, meaning that each service provided to a Medicaid enrollee is reimbursed at an established rate. BHOs, on the other hand, receive a “capitated” payment – or a lump sum based on the number of enrollees – to provide behavioral health services. HCPF announced that the new administrative entities will need to be licensed to bare the financial risk of providing behavioral health services – consistent with how the BHOs currently operate.
HCPF indicates that the ACC and BHO payment approaches will be better aligned over the course of the new five-year contracts. While vague on details, HCPF leaves the door open for different approaches in different regions and to phase in the changes. Most significant, however, is that the announcement represents an alignment of the ACC with a broader theme in health care: the integration of behavioral health and primary care.
These decisions bring up many questions – such as what the new collaborative entities will look like and what payment changes are on the horizon. What is certain is that they represent another phase of Colorado’s changing health policy map.